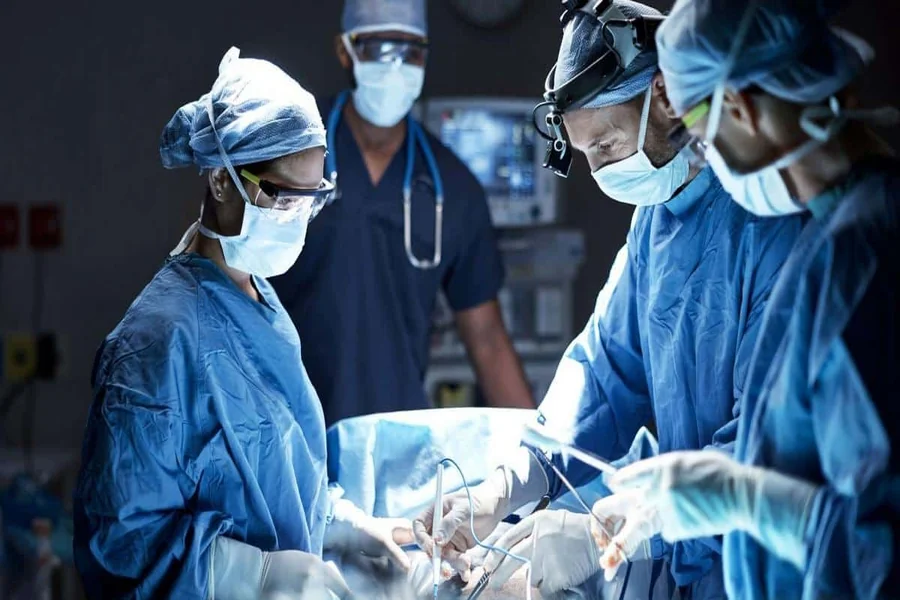
Medical treatment is built on a foundational principle — first, do no harm. When a physician recommends a procedure, patients trust that the recommendation is grounded in sound clinical judgment and genuinely necessary. When that trust is betrayed by a procedure that was never medically warranted, the resulting harm carries a weight that goes beyond the physical injury itself.
Unnecessary medical procedures are recognized as a form of medical malpractice, causing genuine harm to thousands of patients every year. The injuries — surgical complications, anesthesia reactions, infections, permanent organ damage, and lasting psychological trauma — are made more devastating by the knowledge that they were entirely avoidable. Understanding how unnecessary procedures constitute negligence, and what remedies are available in Nevada, is the first step toward accountability.
What Makes a Medical Procedure Legally Unnecessary
A procedure is legally unnecessary when a reasonably competent physician in the same specialty, faced with the same clinical information, would not have recommended it. This reasonable-physician standard is the benchmark in malpractice litigation and requires expert testimony to establish it. The question is not whether the procedure caused harm, but whether the decision to perform it fell below the governing standard of care.
Procedures can be unnecessary for several reasons — misdiagnosis leading to surgery for a nonexistent problem, recommending an invasive intervention when conservative treatment would have sufficed, failing to conduct adequate diagnostic testing, or being influenced by financial incentives that distorted clinical judgment. Each scenario produces the same legal result — a patient subjected to risks they should never have faced — but the investigation required differs by circumstance.
Misdiagnosis as the Gateway to Unnecessary Treatment
The most common pathway to unnecessary procedures is misdiagnosis. A patient incorrectly told they have cancer and who undergoes surgery, chemotherapy, or radiation has been subjected to treatments entirely unjustified by their actual condition. A patient whose imaging is misread and who undergoes spinal surgery for a clinically insignificant abnormality faces permanent risks for a condition that conservative management would have addressed.
These cases are particularly damaging because the patient enters treatment believing they are being helped, delaying recognition of the error. By the time the misdiagnosis is discovered, the procedure may have created new medical problems on top of the underlying condition that was never properly treated. Establishing the misdiagnosis as root cause requires expert testimony explaining both the diagnostic error and the clinical pathway to the unwarranted intervention.
Financial Incentives and the Corruption of Clinical Judgment
Not every unnecessary procedure arises from honest error. Some recommendations are influenced by financial incentives, creating conflicts between the physician’s economic interests and the patient’s medical interests. In systems where compensation is tied to procedural volume rather than outcomes, the incentives to recommend intervention over conservative management can be powerful.
Research has documented regional variations in procedure rates that cannot be explained by patient population differences — variations reflecting financial and systemic influences rather than genuine medical need. Victims working with a reputable medical malpractice law firm in Las Vegas have access to the investigative resources needed to uncover these conflicts and present them as part of a comprehensive negligence case.
The Informed Consent Dimension
A related legal theory frequently arising in these cases is failure of informed consent. Physicians must disclose a procedure’s nature, risks, benefits, alternatives, and consequences of declining — and obtain voluntary agreement. When a procedure is unnecessary, the consent process is corrupted at its foundation, because a patient accurately informed the procedure was unwarranted would not have consented.
Even when a physician believed the procedure was necessary, failure to disclose risks or discuss alternatives can constitute independent liability. Nevada law requires informed consent to be genuine — not merely a signed form, but actual communication giving the patient information needed for an autonomous decision. Victims may have viable informed consent claims in addition to standard negligence claims.
The Harm That Unnecessary Procedures Cause
Physical harm encompasses surgical complications including bleeding, nerve damage, and organ injury; anesthesia reactions ranging from minor effects to life-threatening events; post-operative infections; and lasting functional limitations that major procedures impose regardless of technical success. All of these are made legally actionable by the procedure’s unnecessary nature.
Beyond physical harm, patients who discover they underwent an invasive intervention for no legitimate reason frequently experience profound betrayal, anger, and anxiety that persists long after physical wounds heal. Disruption to work, relationships, and daily life during recovery represents an additional compensable layer. A complete damages analysis must account for all dimensions rather than focusing narrowly on direct medical costs.
Proving the Standard of Care
Establishing that a procedure was unnecessary requires qualified experts who can explain what the standard of care required, how the defendant departed from it, and why a competent physician would not have recommended the procedure. This testimony is the cornerstone of any Nevada malpractice case, and the quality of retained experts is among the most important factors in the outcome.
Finding experts willing to testify, with the specific credentials and clinical experience required, who can communicate complex concepts persuasively to a lay jury is one of malpractice litigation’s most demanding aspects. Defendants retain their own experts to testify the standard was met, creating a battle of opinions the jury must resolve. The preparation and credibility of the plaintiff’s experts relative to the defendant’s is often the decisive factor.
Taking Legal Action in Nevada
Nevada imposes specific procedural requirements on malpractice claims, including a required affidavit of merit from a qualified expert before the case can proceed. The statute of limitations is generally three years from the injury date or one year from discovery, whichever comes first. These deadlines are strictly enforced.
If you’re a malpractice victim, consult an experienced attorney right away. Early help is crucial for case evaluation, evidence preservation, and meeting deadlines. Harm from unnecessary procedures is preventable and shows a failure to provide the care every patient deserves. Nevada law ensures accountability, and victims need skilled representation to pursue their rights.
Passionate about exploring diverse ideas and sharing inspiration, I curate content that sparks curiosity and encourages personal growth. Join me at ElementalNest.com for insights across a wide range of topics.